Everything You Need to Know About Oily Skin

Lifestyle Habits That Cause Acne: The Hidden Diet, Stress and Sleep Triggers (2026)
Medically reviewed • Updated March 2026 • Evidence-based skincare
Lifestyle habits that cause acne—such as diet, stress, and sleep—affect breakouts by increasing oil production, inflammation, and pore congestion. High-glycemic foods raise insulin levels, stress increases cortisol, and poor sleep slows skin repair—creating the conditions for acne to develop over time.
The three main lifestyle triggers of acne include:
- Diet (Morning): High-glycemic foods increase insulin and accelerate sebum buildup inside the pore.
- Stress (Midday): Elevated cortisol levels increase inflammation and make pores more reactive.
- Sleep (Night): Poor sleep slows the skin’s repair cycle, allowing dead skin cells and bacteria to accumulate.
If you want to explore what’s happening inside the pore in more detail, our guide on how acne develops in oily skin throughout the day breaks down the full mechanism. Here, we’ll focus on how everyday habits amplify those signals.
If you tend to notice more breakouts when your routine is off, you’re not imagining it. Understanding how oily and acne-prone skin behaves—and why it naturally produces more oil—helps explain why these daily shifts have such a visible impact on your skin.
Table of Contents
Do Lifestyle Habits That Cause Acne Really Matter for Your Skin?
Lifestyle habits such as high-sugar diets, chronic stress, and poor sleep can increase oil production, inflammation, and slow skin repair. While they don’t directly cause acne, they amplify the biological processes that lead to clogged pores and breakouts—especially in oily, acne-prone skin.
ⓘ Dermatology Note
Acne develops when excess oil, sticky skin cells, bacteria, and inflammation interact inside the pore. Hormones and genetics are the primary drivers, but lifestyle factors—like diet, stress, and sleep—can influence how strongly these processes show up in acne-prone skin.
How Lifestyle Habits Influence Acne Throughout the Day

One of the easiest ways to understand acne is to look at it as something that unfolds throughout your day—not just in a single moment.
Your skin is constantly responding to internal signals and external habits. Some of these are part of your body’s natural rhythm, while others are shaped by your daily routine.
What you eat in the morning can influence oil production. Stress during the day can increase inflammation. And at night, sleep gives your skin a chance to repair and reset.
When sleep is disrupted, that repair process slows down—and breakouts can linger longer than they should.
On their own, these signals might seem small. But together, they can reinforce the conditions that allow acne to develop.
Once you start to see this pattern, it becomes easier to understand how everyday habits affect your skin—and how small changes can help interrupt that cycle.
How Daily Habits Influence Acne Throughout the Day
The table below summarizes how common lifestyle habits influence oil production, inflammation, and skin balance at different times throughout the day.
| Time of Day | Lifestyle Signal | What Happens in the Skin | Effect on Acne |
|---|---|---|---|
| Morning | High-glycemic foods | Insulin and IGF-1 increase oil production | Pores fill with sebum |
| Daytime | Stress | Cortisol increases inflammation | Pimples become irritated |
| Night | Poor sleep | Skin repair slows | Breakouts persist or worsen |
A single meal, stressful day, or late night will not automatically cause acne. However, repeated lifestyle signals can gradually increase the conditions that allow acne to form.
A closer look at how daily habits shape your skin:
Morning Signal: How Diet Influences Oil Production
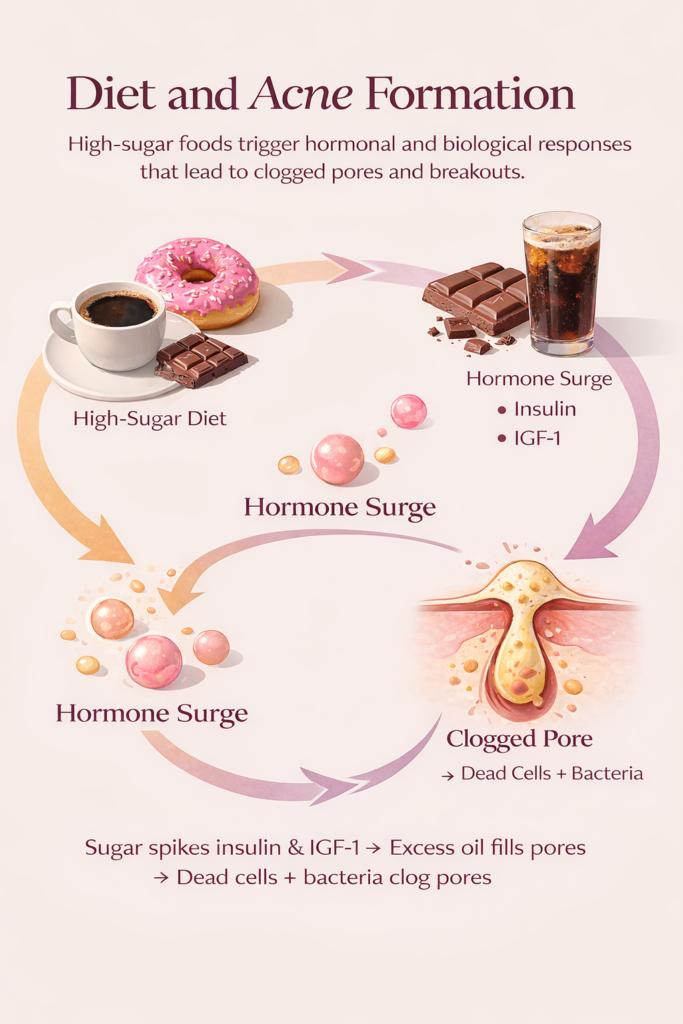
For oily, acne-prone skin, the way your day starts can quietly influence what happens hours later.
And for many people, that interaction begins at the breakfast table.
What you eat in the morning can affect hormones that regulate oil production. Foods that cause rapid blood sugar spikes—like sugary coffee, pastries, or white bread—can trigger a rise in insulin, a connection that has been widely discussed in dermatology research on diet and acne. As insulin increases, the body also produces more insulin-like growth factor-1 (IGF-1).
This relationship between blood sugar, hormones, and oil production is often called the insulin–acne axis.
Think of IGF-1 as a kind of “growth signal.” While it plays an important role in the body, higher levels can also tell sebaceous glands—the tiny oil-producing structures attached to each pore—to produce more sebum.
For oily skin types, this matters. When oil production increases further, pores can fill more easily with sebum and dead skin cells—creating the environment where breakouts begin.
Science Insight
High-glycemic foods don’t directly cause acne, but they can influence the hormonal signals behind it.
Higher insulin and IGF-1 levels may increase oil production and speed up the buildup of skin cells inside the pore—making clogging more likely.
High-Glycemic vs Lower-Glycemic Breakfast Choices
The type of breakfast you choose can influence how strongly these hormonal signals occur during the morning hours.
| High-Glycemic Breakfast | Lower-Glycemic Alternative |
|---|---|
| Sugary latte + pastry | Oats with nuts or seeds |
| White toast with jam | Whole-grain toast with eggs |
| Sweet breakfast cereal | Greek yogurt with berries |
| Fruit juice | Whole fruit and water |
Lower-glycemic foods release energy more slowly, helping maintain steadier blood-sugar levels throughout the morning.
Why This Matters for Oily Skin
Oil production naturally increases during the morning and early afternoon.
When high-glycemic foods trigger additional insulin signaling at the same time, this can amplify the skin’s natural oil production cycle.
Over time, the combination of increased sebum, sticky skin cells, and bacteria inside the pore can contribute to the formation of blackheads, whiteheads, or inflamed breakouts—especially when excess oil remains on the skin long enough to oxidize and thicken within the pore.
Topical ingredients can also help regulate oil production. Our guide on niacinamide for oily skin explains how this ingredient helps reduce the sebum excretion rate in acne-prone skin.
Gentle Glow Insight
Diet is rarely the sole cause of acne, but it can influence how strongly the biological signals behind acne occur.
Balanced meals that include fiber, protein, and healthy fats help support steadier hormone signaling and reduce sudden spikes that may increase oil production.
Daytime Signal: How Stress Amplifies Oil and Inflammation

While diet may set the tone in the morning, stress often becomes the dominant signal as the day unfolds.
Whether it’s work pressure, deadlines, or emotional stress, these moments don’t just affect how you feel—they can also influence how your skin behaves.
This connection happens through a hormone called cortisol, often referred to as the body’s main stress hormone and widely studied in dermatology research for its role in skin inflammation and oil production.
When your brain perceives stress, it activates what’s known as the brain–skin axis—a communication pathway between your nervous system and your skin. Through this pathway, stress signals can directly affect oil production and inflammation.
As cortisol levels rise, sebaceous glands may produce more oil. At the same time, inflammation in the skin can increase, making pores more reactive and sensitive.
For oily and acne-prone skin, this combination can intensify the conditions that allow breakouts to form. Pores that are already filled with oil may become more inflamed, increasing the likelihood that small clogs turn into visible pimples—especially when excess oil builds up and isn’t properly cleared by ingredients that help keep pores refined and balanced.
In practice, this often includes targeted treatments like salicylic acid products that help prevent blackheads from forming throughout the day.
That’s why breakouts often seem to appear during—or right after—periods of stress.
Science Insight
Stress doesn’t directly create acne, but it can amplify the processes behind it.
Higher cortisol levels may increase oil production, trigger inflammatory responses, and weaken the skin’s ability to regulate bacteria inside the pore.
Why Stress Can Worsen Existing Breakouts
Stress rarely creates acne on its own. More often, it builds on what’s already happening beneath the surface.
When pores already contain excess oil and dead skin cells, cortisol-driven inflammation can make these areas more reactive. This increases the likelihood that bacteria inside the pore will trigger visible breakouts.
In this way, stress tends to act as an accelerator rather than the root cause.
What Does Stress Acne Look Like?
Recognizing stress-related breakouts becomes easier once you know what to look for.
Unlike hormonal acne, which often follows a predictable cycle, or diet-related breakouts that may appear as small, uniform bumps, stress acne tends to show up a little differently.
Stress acne doesn’t always look dramatically different—but there are subtle patterns that can help you recognize it.
Deeper, under-the-skin bumps: These breakouts are often more tender and take longer to surface.
Clusters of redness: Because stress increases inflammation, the surrounding skin can appear more flushed or reactive than usual.
Slower healing: Elevated cortisol can delay the skin’s natural repair process, meaning breakouts may linger longer than expected.
Where is Stress Acne Located?
Stress-related breakouts can appear anywhere, but they often show up in areas where the skin is more reactive or where tension tends to build throughout the day.
Common areas include:
Jawline and chin: This area is especially sensitive to internal and hormonal shifts.
Forehead and temples: Often linked to daily tension and stress buildup.
Cheeks: Where inflammation tends to appear more visibly.
The Mind–Skin Connection and the Rise of Neurocosmetics
In recent years, there has been growing interest in the mind–skin connection—and what’s now often referred to as neurocosmetics.
This approach focuses on how emotional and neurological signals influence skin behavior. The idea is simple: your skin doesn’t just respond to what you apply topically—it also responds to what your body is experiencing internally.
Instead of only treating breakouts after they appear, this perspective encourages addressing the signal at its source.
Small habits—like taking short breaks, staying hydrated, or incorporating moments of relaxation—can help reduce prolonged stress signals that influence oil production and inflammation.
Nighttime Signal: How Sleep Supports Skin Repair

As the day winds down, your skin shifts into a different mode—one focused on repair and recovery.
During sleep, the body supports some of the skin’s most important functions, including barrier repair, inflammation regulation, and healthy cell turnover.
For oily and acne-prone skin, this nighttime phase plays a key role in restoring balance inside the pore.
When sleep is limited or inconsistent, that recovery process becomes less efficient. The body may remain in a more activated, stress-like state, and the skin doesn’t get the full opportunity to reset.
At the same time, the skin barrier repairs more slowly. When this barrier is compromised, the pore environment becomes more vulnerable to irritation and bacterial imbalance.
Over time, this can make breakouts feel more persistent—and slower to heal.
Science Insight
Deep sleep supports the biological processes that keep skin balanced.
During this phase, the body helps regulate hormones, strengthen the skin barrier, and reduce inflammatory signals. When sleep is disrupted, these processes may become less effective, allowing irritation and acne-related inflammation to linger.
Research from the National Institutes of Health (NIH) and recent 2026 clinical data show that “poor sleepers” experience a 50% slower recovery rate in their skin barrier compared to those who get deep rest.
Why Sleep Matters for Acne-Prone Skin
Sleep plays a quiet but important role in maintaining skin balance.
At night, the body supports processes like barrier repair, inflammation control, and healthy cell turnover—especially when supported by a simple nighttime routine that helps the skin recover and maintain balance. When sleep is shortened or inconsistent, these processes become less efficient.
As a result, irritation can linger longer in the skin, allowing clogged pores and inflammation to persist—and making breakouts more likely to develop or take longer to resolve.
The 24-Hour Lifestyle Acne Cycle
From what we’ve discussed, your daily habits don’t just happen in isolation—they work together to shape how acne develops over time.
Think of it as a flow that builds throughout the day. It often begins in the morning, where a high-sugar breakfast can increase insulin levels and signal your oil glands to produce more sebum. As the day progresses, stress can layer on top of that, raising cortisol levels and making the skin more reactive and inflamed.
By nighttime, your skin shifts into repair mode. This is when it’s meant to reset and recover—but if sleep is disrupted, that process becomes less effective, allowing irritation and breakouts to carry over into the next day.
Rather than acting separately, these signals build on one another—creating a cycle that can gradually reinforce acne.
Lifestyle Habits That Help Support Clear Skin
You don’t need a perfect routine to support your skin—just more consistent, balanced signals throughout the day.
Starting with your mornings, small shifts in what you eat—and protecting your skin daily without triggering breakouts—can make a noticeable difference.
Choosing lower-glycemic options like oats, eggs, or berries—and building a routine that helps control oil throughout the day—can support steadier hormone signaling and reduce sudden spikes that influence oil production.
As the day goes on, stress becomes just as important to manage. Even short pauses—like stepping away from your screen, taking a walk, or slowing your breathing—can help regulate your body’s stress response. These small resets can reduce prolonged cortisol signals that may otherwise make the skin more reactive.
At night, your focus shifts to recovery. Sleep isn’t separate from skincare—it’s part of it. Maintaining a consistent sleep schedule and limiting late-night screen exposure can help support the skin’s natural repair process and allow it to reset more effectively.
Alongside these habits, your skincare routine plays a supporting role. Using gentle, non-comedogenic products—like choosing a cleanser that won’t strip your skin barrier and supporting hydration without clogging pores—and ingredients like niacinamide can help regulate oil production and support the skin barrier, making pores less likely to become congested.
Common Lifestyle Mistakes That Worsen Acne
Some habits can unintentionally reinforce the acne cycle:
The sugar–caffeine loop: Using sugary drinks to compensate for fatigue can create repeated spikes in both insulin and stress signals.
Late-night screen use: Blue light exposure can interfere with the body’s natural sleep rhythm, affecting the skin’s repair phase.
Post-workout neglect: Allowing sweat and oil to sit on the skin for too long can contribute to clogged pores.
Conclusion: How Daily Habits Shape Acne Formation
Acne is more than just “dirty skin” or “bad luck.” It is a biological response to a series of daily lifestyle signals. By understanding the Morning-Day-Night cycle, you can move from reacting to breakouts to preventing them at the source.
Understanding the lifestyle habits that cause acne gives you more control over how your skin behaves day to day.
Your skin is constantly listening. Today, what signals are you sending?
Frequently Asked Questions: Lifestyle & Acne
Why do I get pimples when I don’t sleep enough?
When you skip sleep, your body stays in a state of high alert. This causes cortisol (the stress hormone) to stay elevated throughout the night instead of dropping. This elevated cortisol signals your oil glands to produce more sebum while simultaneously slowing down your skin’s repair process. Essentially, you’re waking up with more oil and less “cleanup” than your skin needs.
Where is stress acne located?
Stress acne often follows a pattern but can be more widespread than cyclical hormonal acne. You will typically find stress-related breakouts on the forehead, temples, and cheeks, where oil glands are highly concentrated. However, it can also appear along the jawline if the stress is chronic and begins to affect your overall hormonal balance.
What does stress acne look like?
Stress acne is usually inflammatory. Unlike a simple blackhead, stress-induced pimples tend to be red, swollen, and sometimes tender to the touch. They often appear as clusters of small red bumps or deeper, painful “under-the-skin” cysts that take much longer to heal than typical breakouts.
Can lifestyle habits actually cause acne?
In 2026, we view lifestyle habits as “biological amplifiers.” While genetics and hormones are the root cause, habits like a high-sugar diet, chronic stress, and poor sleep send signals that tell your acne-prone skin to produce more oil and more inflammation. These are often described as lifestyle habits that cause acne, not by creating it directly, but by amplifying the signals behind breakouts. By changing these habits, you aren’t just “cleaning” your skin; you are changing the internal messages your skin receives.
How can I stop oily skin overnight?
While you can’t change your genetics overnight, you can support your nighttime repair. Focus on Sleep Hygiene (keeping a cool room and avoiding blue light) to ensure your cortisol drops. Topically, using ingredients like Niacinamide or a lightweight, non-comedogenic moisturizer —and understanding how different acne treatments work for oily skin—can help regulate oil production and prevent excess buildup.
Can diet affect oily skin and breakouts?
Yes, certain foods—especially those that cause rapid blood-sugar spikes—can influence hormones linked to oil production. This may increase sebum levels in the skin and contribute to clogged pores in acne-prone individuals.
Medical Disclaimer
Gentle Glow guides are developed using peer-reviewed dermatology research and established clinical guidelines. The information provided is for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. Always consult a board-certified dermatologist or qualified healthcare provider before starting new active skincare treatments.
This article is based on dermatology research and peer-reviewed studies on acne pathogenesis, hormonal signaling, and skin barrier function.
Sources and References
- National Institutes of Health (NIH). Diet and Acne: The Role of Glycemic Load and Hormonal Signaling.
Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC8971946/ - Journal of the American Academy of Dermatology (JAAD). Stress and Acne: The Role of Cortisol in Skin Inflammation and Sebum Production.
Available at: https://www.jaad.org/article/S0190-9622(14)00023-1/abstract - ScienceDaily. High Glycemic Diet Linked to Acne Development Through Hormonal Pathways.
Available at: https://www.sciencedaily.com/releases/2013/07/130723155002.htm



