Everything You Need to Know About Oily Skin

How to Fix a Damaged Skin Barrier from Over-Exfoliation (2026 Guide for Oily and Acne-Prone Skin)
Gentle Glow Editorial Team • Updated April 2026 • Evidence-based skincare
Knowing how to fix a damaged skin barrier requires stopping all active treatments immediately to restore the lipid layer, as disruption increases transepidermal water loss (TEWL) and triggers excess oil production. By following a barrier-repair routine, you can calm sensitivity without worsening breakouts. In 2026, dermatology focuses on non-comedogenic lipid repair to restore stability in oily, acne-prone skin.
- Stop BHAs, AHAs, retinoids, and scrubs immediately.
- Use a gentle cleanser, a non-comedogenic moisturizer, and daily mineral SPF.
- Allow at least 7 days for visible calming and up to 28 days for full recovery.
Table of Contents
Quick Video Guide: How to Fix a Damaged Skin Barrier
Why over-exfoliated skin feels so confusing
A damaged skin barrier does not always look the way people expect.
Most online advices describe barrier damage as red, flaky, dry skin. That can happen, but oily and acne-prone skin often behaves differently. Instead of looking obviously dry, it can look shinier than usual. Your face may feel tight after cleansing, yet still become greasy a few hours later. It may look smooth from a distance, but feel irritated, rough, or strangely fragile up close.
That is what makes this kind of skin damage so confusing.
Many people assume the extra shine means their skin is still oily. Others think the smooth, reflective look means their products are working. But when your barrier has been over-exfoliated, that shine is often not a healthy glow at all. It is a stressed surface that is no longer holding moisture properly.
This pattern becomes much clearer when you understand how oily skin actually behaves at a deeper level, which we explain in our guide to how oily and acne-prone skin actually behaves.
This is especially common if you have been using too many actives too often, like exfoliating acids or retinoids. If that sounds familiar, it helps to think of this less as a “bad skin week” and more as a barrier crash.
And once that crash happens, your skin stops behaving normally.
What the skin barrier actually is
Your skin barrier, often referred to as the outer layer of the skin, is a complex, structured system—not just a simple layer of “dead skin.” It functions as a protective seal made of skin cells and lipids, including ceramides, cholesterol, and fatty acids.
These components work together to help your skin retain water, stay resilient, and protect itself from external irritation. When this structure is intact, your skin feels balanced, stable, and “plastic” (meaning it moves and stretches without cracking).
When Function Fails: The TEWL Cascade
When this structure is disrupted through over-exfoliation, everything becomes less predictable. It is no longer just a “dryness” issue; it is a fundamental loss of function.
Water escapes more easily through a process called transepidermal water loss (TEWL), which causes the skin to lose its “plasticity” and become rigid or tight. This process is extensively detailed in clinical research on barrier integrity, which demonstrates that water loss acts as a “biosensor” trigger.
When your skin “leaks” water, it sends an emergency signal that kickstarts an inflammatory response—often described as a disruption in barrier function and increased sensitivity (as outlined by the American Academy of Dermatology).
That is why barrier damage is not just about dryness. It is about a biological system in crisis.
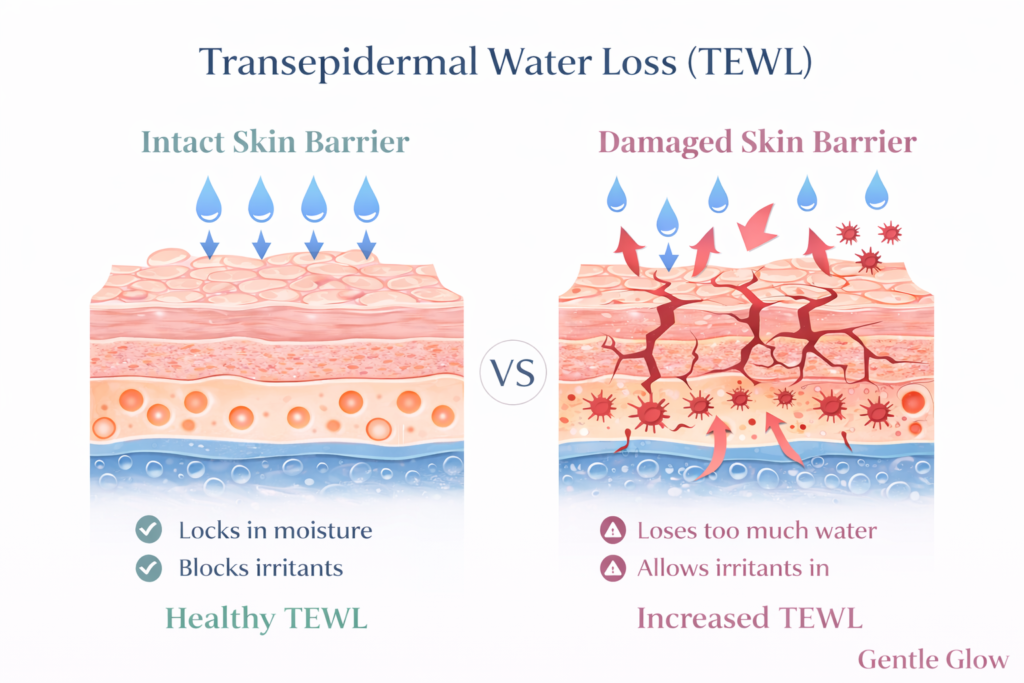
What over-exfoliation does to the skin
Exfoliation can be helpful when used correctly. It helps remove buildup and supports smoother skin. But when it is overused, it starts to damage the very structure it is meant to improve.
When you over-exfoliate, you begin to strip away the lipids that hold the skin barrier together. This weakens the structure of the outer layer and increases transepidermal water loss (TEWL), meaning your skin loses hydration faster than it can retain it.
As this happens, your skin starts to feel tight, sensitive, and reactive.
At the same time, oily skin often responds by producing more sebum. This creates a confusing situation where the skin is dehydrated underneath but oily on the surface. Instead of feeling balanced, it feels unstable.
This is also why overusing actives like salicylic acid or retinoids can backfire when not balanced properly. If you want to understand how these ingredients work when used correctly, you can read more in our guide on salicylic acid for oily and acne-prone skin and how retinoids regulate cell turnover over time.
Why oily skin can look shiny but feel tight
This is one of the most overlooked signs of barrier damage.
When the surface of the skin becomes over-exfoliated, it loses some of its natural texture and starts reflecting light in a harsher, flatter way. This is what creates that “waxy” or overly shiny appearance. It may look smooth, but it is not a healthy glow.
At the same time, the barrier is losing water.
So while the surface appears oily, the skin underneath is dehydrated. This is what creates that tight feeling after cleansing and the sensitivity when applying products.
This pattern is closely linked to what we explain in our guide on dehydrated oily skin, where oil and water imbalance exist at the same time.
The result is a combination of:
- shine
- tightness
- rough or sandpaper-like texture
- increased sensitivity
And because this combination is not widely explained, many people misinterpret what their skin is trying to tell them.
Why breakouts can get worse after over-exfoliation
Breakouts often increase after over-exfoliation because the skin loses its ability to regulate what happens inside the pore.
When the skin barrier is disrupted, transepidermal water loss (TEWL) rises and the skin becomes dehydrated. In response, sebaceous glands increase oil production to compensate. This excess oil mixes with unevenly shed skin cells, creating a higher chance of buildup inside the follicle.
At the same time, barrier damage triggers low-level inflammation. This makes the pore environment more reactive and easier to disrupt, allowing early clogs to progress more quickly into visible breakouts. This pattern is commonly seen in how deeper acne forms in oily skin, where inflammation develops beneath the surface and becomes harder to control.
This is why acne can worsen even when you are using “acne-fighting” ingredients. The issue is no longer just clogged pores—it is an unstable skin environment.
This mechanism is closely linked to how acne forms at its earliest stage, which we explain in detail in our guide on what causes acne on oily skin and the full formation cycle.
At this stage, adding more exfoliation usually increases irritation and delays recovery. Restoring barrier function allows oil flow, cell turnover, and inflammation to return to a more stable pattern.
How to tell if your skin barrier is damaged
If your skin suddenly feels different and you are not sure why, there are a few patterns that usually point to barrier damage.
The most common sign is that your skin feels both oily and tight at the same time. Another is when products that never used to bother you start to sting, including cleanser or moisturizer. Some people also notice that their skin looks unusually shiny or waxy, but feels rough to the touch.
Breakouts may become more inflamed, and the overall skin feels more sensitive than usual.
What matters is the combination of these signs.
When shine, tightness, stinging, rough texture, and sensitivity all appear together—especially after using strong actives—this usually indicates that the skin barrier has been disrupted.
The 7-day reset: how to fix a damaged skin barrier after over-exfoliation
The first step in how to fix a damaged skin barrier is not adding more products, but removing what is disrupting it. A short reset period allows the skin to reduce transepidermal water loss (TEWL) and stabilize before deeper repair begins.
Days 1–3: Stop the damage and calm the skin
At this stage, the goal is to reduce irritation and prevent further water loss.
Keep your routine minimal. Use a gentle, non-stripping cleanser or rinse with water, followed by a lightweight moisturizer that supports the skin barrier without clogging pores. Avoid all exfoliating acids, retinoids, and strong treatments.
The skin may still feel tight, sensitive, or unusually shiny during these days. This is expected, as the barrier is still compromised and TEWL remains elevated.
Days 4–7: Support lipid repair and restore balance
Once irritation begins to settle, the focus shifts to rebuilding the skin’s lipid matrix.
Continue using a non-comedogenic moisturizer, but now prioritize ingredients like ceramides, cholesterol, and fatty acids, along with soothing agents such as panthenol or cica. These help reinforce the barrier structure and improve water retention.

As hydration improves, the skin gradually becomes less tight and less reactive. Oil production also starts to stabilize, reducing that shiny but uncomfortable feeling.
The 21-day repair phase: how to fix a damaged skin barrier by rebuilding strength
While the first week focuses on calming the skin, full repair takes longer.
The skin barrier follows a natural renewal cycle of around 21 to 28 days. During this time, new skin cells form and the lipid structure continues to rebuild.
Consistency matters more than intensity here.
Maintain the same simplified routine, continue avoiding strong actives, and focus on supporting barrier function daily. Introducing new products too early can interrupt this process and prolong recovery.
When to reintroduce active ingredients
Returning to actives too soon is one of the most common reasons barrier damage repeats.
Before reintroducing ingredients like salicylic acid or retinoids, your skin should feel stable—not just look better. This means no stinging, reduced sensitivity, and a more balanced oil level.
A simple way to assess this is how your skin reacts to basic products. If a gentle moisturizer or even water still causes discomfort, the barrier is not ready.
Once your skin is stable, you can gradually return to a structured routine. This is where a balanced morning routine for oily acne-prone skin and a well-paced night routine for oily and acne-prone skin become important, allowing you to reintroduce actives without disrupting the barrier again.
When restarting, keep frequency low and allow recovery days between treatments, especially with ingredients that affect cell turnover, such as retinoids, which we cover in detail in our guide on retinoids for oily skin.
Why this reset works for oily, acne-prone skin
Barrier repair does not slow progress—it corrects the conditions that cause instability.
By reducing TEWL, restoring the lipid layer, and calming inflammation, the skin becomes more predictable. This allows oil flow, cell turnover, and pore behavior to normalize.
As a result, breakouts become less reactive, and treatments become more effective when reintroduced later.
What actually repairs a damaged skin barrier
Barrier repair is not about adding more hydration—it is about restoring the lipid structure that holds the skin together.
The outer layer of the skin depends on a balance of ceramides, cholesterol, and fatty acids, a structure well documented in dermatology research on barrier repair. These lipids form the structure that reduces transepidermal water loss (TEWL) and keeps the skin stable.
When this structure is disrupted, applying water-based products alone is not enough. The skin needs lipids to rebuild that structure and regain its ability to retain moisture.
This is why barrier repair focuses on restoring the lipid matrix, not just increasing hydration.
The best ingredients for barrier repair (without clogging pores)
For oily and acne-prone skin, the goal is to repair the barrier without disrupting sebum flow or creating buildup inside the pore.
Instead of layering multiple products, focus on a few ingredients that support barrier function while remaining non-comedogenic.
| Ingredient | What it does for the skin barrier | Why it works for oily skin |
|---|---|---|
| Ceramides | Rebuild the lipid structure and reduce transepidermal water loss (TEWL) | Restore barrier without adding heaviness |
| Panthenol (Vitamin B5) | Supports healing and reduces sensitivity | Lightweight and calming, suitable for reactive skin |
| Squalane | Mimics natural lipids and improves skin flexibility | Absorbs easily without clogging pores |
| Centella Asiatica (Cica) | Reduces inflammation and improves skin tolerance | Helps calm breakouts without adding oil |

These ingredients work together to restore the lipid matrix, improve skin tolerance, and support recovery without triggering congestion.
The niacinamide question (and why less is more)
Niacinamide is often recommended for barrier repair, but concentration matters.
At lower levels (around 2–5%), niacinamide supports ceramide production and helps improve barrier function. It can also help regulate oil production, which makes it useful for oily skin.
At higher concentrations (10% and above), it can become irritating—especially when the barrier is already compromised.
If your skin is still stinging or reactive, it is better to wait before reintroducing it. Barrier repair should reduce irritation, not add another variable.
If you want a deeper breakdown, we cover this in our guide on niacinamide for oily skin.
What to avoid during barrier repair
During recovery, the goal is to reduce stress on the skin.
Avoid exfoliating acids (AHAs, BHAs), retinoids, and strong vitamin C formulations until the barrier has stabilized. These ingredients increase cell turnover or penetration, which can prolong irritation when the barrier is already weakened.
Also avoid over-cleansing or using harsh, foaming cleansers that strip the skin further.
Barrier repair works best when the skin is left undisturbed long enough to rebuild.
Non-comedogenic barrier repair (the oily skin approach)
Heavy occlusive products can feel suffocating on oily skin and may lead to congestion.
Instead of thick balms, focus on lightweight barrier-repair textures such as emulsions, gels, or fluid creams that deliver lipids without blocking pores.
This approach supports repair while maintaining normal sebum flow, which is essential for preventing new clogs.
The goal is not to “seal” the skin aggressively, but to support it in a way that matches how oily skin behaves.
Purging vs. barrier damage: how to tell the difference
Not every breakout after using actives means your skin is purging. The difference comes down to what is happening inside the pore versus what is happening to the skin barrier.
| Pattern | What is happening | How it looks | What it means |
|---|---|---|---|
| Purging | Increased cell turnover brings existing microclogs to the surface faster | Breakouts appear in usual areas and resolve more quickly | Skin is adjusting to the treatment |
| Barrier damage | Disrupted lipid structure → increased TEWL and inflammation | Stinging, tightness, unusual shine, breakouts in new areas | Skin is irritated and unstable |
Purging is limited to areas where you normally break out and does not involve persistent sensitivity. Barrier damage affects the entire skin surface and is usually accompanied by tightness, reactivity, or discomfort when applying products.

If your skin feels irritated, not just congested, it is not purging—it is a sign that the barrier needs repair before continuing treatment.
How to safely return to active ingredients
Reintroducing actives should be gradual and based on how your skin feels, not just how it looks.
Start with low frequency and allow recovery time between applications. Watch for signs of irritation, not just breakouts.
A useful checkpoint is how your skin reacts to simple products. If there is still stinging, tightness, or unusual sensitivity, the barrier is not fully ready.
Once stable, actives can be reintroduced in a controlled way, supported by a consistent routine that helps maintain progress without triggering another cycle of damage.
Final takeaway: what actually fixes a damaged skin barrier
Learning how to fix a damaged skin barrier is less about adding more products and more about restoring how your skin functions.
Once transepidermal water loss (TEWL) is reduced and the lipid structure begins to recover, the skin becomes more stable. Oil production, sensitivity, and breakouts start to regulate naturally instead of reacting unpredictably.
For oily and acne-prone skin, this step is essential.
Treatments work better when the barrier is intact. Without that stability, even the right ingredients can lead to more irritation instead of improvement.
The goal is not to push your skin harder, but to support it until it can regulate itself again.
Frequently Asked Questions
How to repair a damaged skin barrier for oily, acne-prone skin quickly?
To repair the barrier quickly, you must adopt a “skinimalist” routine immediately. This means stopping all BHA, AHA, and retinoids for at least 7 to 14 days. Focus on a pH-balanced cleanser and a ceramide-dominant moisturizer. While you cannot “fix” a barrier overnight, you can stop the stinging and inflammatory response within 24–48 hours by sealing the skin with a non-comedogenic lipid balm.
Can I use niacinamide serum on a damaged skin barrier?
Yes, but the concentration is critical. At levels of 2% to 5%, niacinamide actually helps heal the barrier by stimulating natural ceramide production. However, 10% or 20% serums can act as an irritant on a “broken” barrier. If your skin stings upon application, stop the serum and wait until your skin passes the Neutral Skin Test (no stinging with plain water or basic moisturizer).
Why is my skin more oily now that it’s damaged?
This is known as rebound sebum production. When your barrier is compromised, your skin loses water rapidly through transepidermal water loss (TEWL). In a “panic” response to prevent complete dehydration, your sebaceous glands produce excess oil to try and create a makeshift seal. This is why over-exfoliated skin often feels tight but looks waxy or shiny.
How long until over-exfoliated skin heals completely?
While you will see a reduction in redness and stinging within 7 days, full structural repair of the lipid matrix takes 21 to 28 days. This timeline matches your natural skin cell turnover cycle. You should not reintroduce high-strength actives (like Acretin or 2% BHA) until you have completed a full 28-day cycle of consistent, irritant-free repair.
How can I tell if I am purging or if my barrier is damaged?
The difference is found in location and sensation:
Purging: Breakouts occur only in your “usual” spots and do not cause stinging or persistent redness.
Barrier Damage: Breakouts appear in new areas, and the skin feels tight, sensitive, or “raw.” If your basic moisturizer or sunscreen stings, you are dealing with barrier damage, not a purge.
What is the best non-comedogenic barrier repair moisturizer?
The best repair cream for oily skin should contain the “Big 3” lipids: Ceramides, Cholesterol, and Fatty Acids, but in a lightweight, gel-cream or emulsion texture. Look for ingredients like Squalane (which mimics human sebum) and Panthenol (Vitamin B5) to calm the “fire” of inflammation without blocking pores or causing new cystic acne.
Sources and References
- Journal of Clinical Investigation. Aquaporins and skin barrier function.
Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC3396453/ - American Academy of Dermatology (AAD). Moisturizer: Why you may need it if you have acne.
Available at: https://www.aad.org/public/diseases/acne/skin-care/moisturizer - Schild J, Kalvodová A, Zbytovská J, Farwick M, Pyko C. The role of ceramides in skin barrier function and the importance of their correct formulation for skincare applications. International Journal of Cosmetic Science.
Available at: https://pubmed.ncbi.nlm.nih.gov/39113291/
This article is based on dermatology research and peer-reviewed studies on acne pathogenesis, hormonal signaling, and skin barrier function.
Medical Disclaimer
Gentle Glow guides are developed using peer-reviewed dermatology research and established clinical guidelines. The information provided is for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. Always consult a board-certified dermatologist or qualified healthcare provider before starting new active skincare treatments.



