Everything You Need to Know About Oily Skin

Retinoids for Oily Skin: Clear Pores and Prevent Acne (Beginner to Advanced Guide)
Gentle Glow Editorial Team • Updated April 2026 • Evidence-based skincare
Retinoids for oily skin are the gold-standard treatment because they regulate cell turnover, prevent microcomedones, and normalize follicular hyperkeratosis. Unlike surface treatments, they work inside the pore to stop clogs before they form, helping reduce breakouts and keep pores clear with consistent use.
- Prevent early pore clogging (microcomedones).
- Regulate how skin sheds inside the follicle.
- Support long-term acne control, not just short-term fixes.
Table of Contents
Watch: How retinoids work for oily skin (quick explanation)
What are retinoids and how do they work for oily skin?
Retinoids are a group of vitamin A–derived ingredients that help regulate how the skin renews itself, a mechanism widely described in dermatology resources. While they’re often associated with anti-aging, their role in oily and acne-prone skin is more foundational — they influence what happens inside the pore, not just how the surface looks.
Instead of allowing dead skin cells to build up and mix with oil, retinoids help the skin shed more evenly. This keeps the pathway inside the pore clearer, which is where most breakouts actually begin.
For oily skin, this matters more than simply reducing shine.
Excess oil on its own isn’t the problem — it’s how that oil interacts with dead skin cells. When that process becomes uneven, buildup forms, pores appear larger, and breakouts repeat in the same areas — something we break down in detail in our guide on what causes acne on oily skin and how it develops over time.
Retinoids work by gradually correcting that pattern.
Over time, this leads to smoother texture, fewer recurring clogs, and more stable oil flow — which is why retinoids are often used not just to treat acne, but to change how acne forms in the first place.
If you’re building your routine from the ground up, this fits into the bigger picture of how oily and acne-prone skin behaves and what it actually needs to stay balanced.
Why most products stop working after a few days
Most skincare products fail because they treat the surface, not the source of the clog.
If you have oily skin, you’ve likely seen this pattern — temporary improvement followed by the same congestion returning.
The shine comes back. The pores refill. The bumps reappear.
That’s because most products act on what’s already visible.
Retinoids work earlier in the cycle.
Instead of clearing what you see, they prevent the buildup that leads to it. This is why guidance from the American Academy of Dermatology acne guidelines includes topical retinoids as a core treatment for acne-prone skin.
But effectiveness depends on how they are used.
Retinoids require consistency, gradual introduction, and barrier support. When used too aggressively, they can lead to irritation, which disrupts the skin and can actually increase oil imbalance.
The goal is to guide your skin into a more stable, predictable pattern over time.
Why retinoids for oily skin work differently
Retinoids improve how oil moves through the pore by preventing buildup at its source.
Oily skin isn’t just about producing more sebum — it’s about how that sebum flows. This behavior is closely tied to how pores actually work and why they appear larger in oily skin.
When everything is working normally, sebum flows out smoothly and helps keep the skin balanced. But in acne-prone skin, that flow becomes uneven. Oil mixes with dead skin cells, and instead of exiting the pore, it starts to build up.
This is where most routines focus on the surface — cleansing more, exfoliating more, trying to “remove” the problem after it appears.
Retinoids take a different approach.
Instead of chasing the clog, they help prevent it from forming in the first place.
They do this by improving how the inner lining of the pore sheds and renews itself. Over time, this makes it harder for buildup to stay trapped — which is why pores begin to look clearer and breakouts become less frequent.
What happens inside the pore (and where retinoids step in)
Acne begins before you can see it — and retinoids act at that invisible stage.
Inside the pore, dead skin cells can become slightly adhesive instead of shedding cleanly. When combined with oil, they begin forming early blockages known as microcomedones.
These are the starting point of:
- blackheads
- whiteheads
- inflammatory acne
Retinoids reduce this process at its earliest stage.
Clinical research on topical retinoids shows their role in reducing microcomedone formation and normalizing follicular turnover.
They help normalize how cells shed inside the follicle, preventing them from sticking together and forming the base of a clog. As this process improves, oil flows more freely and the frequency of congestion decreases.
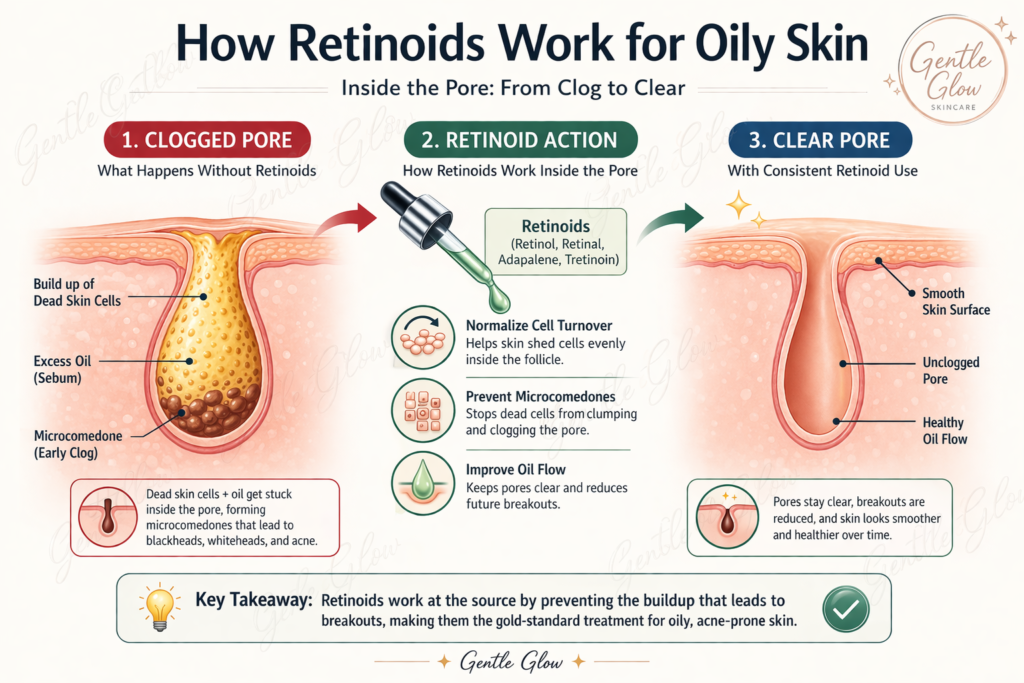
Understanding this stage also helps clarify the difference between blackheads and sebaceous filaments and how they form inside the pore, which often get confused but behave very differently.
Follicular hyperkeratosis — the “sticky cell” problem
Recurring clogged pores don’t start with oil — they start with how skin cells fail to shed inside the pore.
In oily and acne-prone skin, the shedding process becomes uneven. Instead of separating and exiting smoothly, dead skin cells cling together and remain inside the follicle.
This process is called follicular hyperkeratosis — but in simple terms, it’s just:
skin cells that don’t let go when they should
When these cells mix with sebum, they form the base of a clog. Over time, that buildup can oxidize into a blackhead or develop into an inflamed breakout — something closely linked to why skin oil turns dark and how sebum oxidation affects pore appearance.
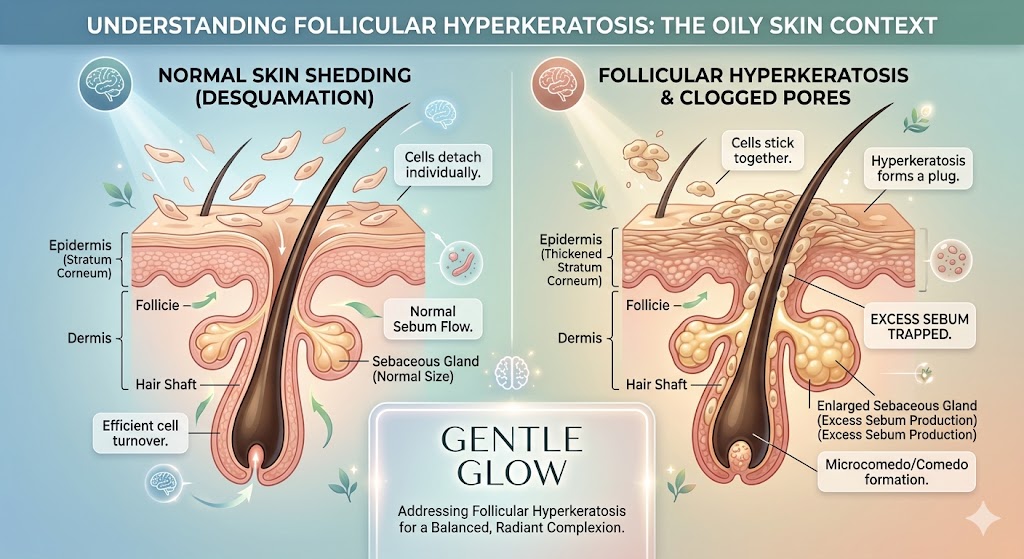
Retinoids target this exact issue.
They don’t force aggressive peeling. Instead, they gradually normalize cell turnover, helping skin shed more evenly so buildup doesn’t form as easily in the first place.
This is also why ingredients like salicylic acid for oily and acne-prone skin can help loosen existing buildup — but through a different mechanism. Retinoids work earlier, before the clog fully develops.
Why most retinoid routines fail for oily, acne-prone skin
Retinoids don’t fail because they’re ineffective — they fail when the skin is pushed faster than it can adapt.
The most common mistake is treating them like a quick solution instead of a long-term adjustment.
Starting too frequently, using too much product, or combining multiple active ingredients can overwhelm the skin. This leads to irritation, which disrupts the barrier and often results in more instability — not less.
Another issue is layering retinoids with strong exfoliants or acne treatments in the same routine.
While these ingredients can work well together, they need to be used strategically. The most effective approach is using them on alternate nights, allowing the skin to benefit from each without increasing irritation or compromising the barrier — something that becomes much easier when you follow a structured night routine for oily and acne-prone skin that balances treatment and recovery.
Retinoids require a transition phase.
The skin needs time to adjust to increased cell turnover, rebuild its barrier, and stabilize oil behavior. Without that adjustment, even well-formulated products can feel too harsh.
The Vitamin A Ladder: from beginner to advanced
Retinoids deliver better results when used progressively — not by jumping straight to the strongest option.
| Stage | Type of Retinoid | Typical Strength | Best For |
|---|---|---|---|
| Beginner | Adapalene / Retinol | 0.1% / 0.3% | Active acne, early congestion |
| Intermediate | Retinal (Retinaldehyde) | 0.05% – 0.1% | Faster results, smoother texture |
| Advanced | Tretinoin / Tazarotene | 0.025% – 0.1% | Persistent acne, long-term control |
Each level reflects how directly the ingredient acts on the skin.
At the beginner stage, the focus is tolerance — allowing the skin to adjust to increased cell renewal without irritation.
At the intermediate stage, improvements become more visible, especially in texture, clarity, and post-acne marks.
At the advanced stage, retinoids are used more strategically for long-term control of persistent acne and deeper congestion.
Moving too quickly between levels often leads to irritation.
Staying consistent at a level your skin tolerates well leads to more stable, long-term results.
Retinol vs retinal vs adapalene vs tretinoin
Not all retinoids work at the same speed — the key difference is how directly they convert into active vitamin A inside the skin.
| Retinoid | Conversion Level | Strength | Best For | Skin Type Fit |
|---|---|---|---|---|
| Retinol | Multiple steps | Mild–moderate | Beginners, texture, early congestion | Sensitive, first-time users |
| Retinal (Retinaldehyde) | One step away | Moderate–high | Faster results, post-acne marks | Oily, tolerant skin |
| Adapalene | Already active (acne-specific) | Moderate | Clogged pores, recurring acne | Oily, acne-prone skin |
| Tretinoin | Fully active | High | Persistent acne, long-term control | Resistant, experienced users |

If you’re unsure where to start, this progression helps you match the right retinoid to your skin’s current tolerance — not just your end goal.
All retinoids belong to the same vitamin A family, but what makes them different is how directly they act on the skin — and how your skin responds to them over time.
At the simplest level, they all aim to do the same thing: improve cell turnover, keep pores clear, and reduce the formation of acne. The difference is in how many steps they need to become retinoic acid, the active form your skin actually uses.
Retinol is the most common starting point. It goes through multiple conversion steps before becoming active, which makes it slower and generally gentler. This is why it’s often used for beginners or for improving overall skin texture and early congestion without overwhelming the skin.
Retinal (retinaldehyde) sits one step closer to the active form. Because of this, it works faster than retinol and tends to show results sooner, especially when it comes to smoothing texture and improving post-acne marks (PIH). It’s often a good next step when your skin is already comfortable with active ingredients.
Adapalene works differently. It doesn’t rely on the same conversion process and is designed specifically for acne-prone skin. It targets clogged pores, microcomedones, and recurring breakouts more directly, which is why it’s often the most practical starting point for oily skin rather than traditional retinol.
Tretinoin is the fully active form — no conversion needed. It works more directly and more powerfully on cell turnover, which is why it’s used for persistent acne and long-term skin regulation. But with that strength comes a higher chance of irritation, so it’s usually introduced gradually and often with medical guidance.
What matters isn’t which one is “strongest,” but how your skin responds to it.
A slower option like retinol can still deliver results if used consistently, while a stronger option like tretinoin can backfire if introduced too quickly. For oily and acne-prone skin, the goal is to choose a retinoid that improves pore behavior, skin renewal, and oil flow without disrupting the barrier — because once the barrier is compromised, oil regulation becomes less stable, not more.
Which retinoid is best for oily, acne-prone skin?
The best retinoid is not the strongest one — it’s the one your skin can tolerate consistently without irritation.
For most people with oily, acne-prone skin, starting with adapalene (0.1%) is often the most practical approach. Unlike traditional retinol, adapalene is designed specifically to target clogged pores, microcomedones, and recurring breakouts, which makes it more directly aligned with how acne develops.
It also tends to be more stable and less irritating than older retinoids, which means your skin is more likely to stay consistent with it — and consistency is what drives results.
If your main concern is persistent congestion, frequent breakouts, or uneven texture, adapalene usually offers the best balance between effectiveness and tolerance.
As your skin becomes more stable, you can then consider moving to retinal (retinaldehyde). Because it converts more efficiently into retinoic acid, it works faster on cell turnover, making it a stronger option for improving texture and post-acne marks (PIH).
The goal is not to jump to the most powerful option.
It’s to choose the one your skin can adapt to — and continue using long enough to actually change how breakouts form over time.
Retinal vs retinol for acne and texture
Retinal works faster than retinol because it converts more directly into active vitamin A inside the skin.
| Feature | Retinol | Retinal (Retinaldehyde) |
|---|---|---|
| Conversion steps | Multiple | One step away |
| Speed of results | Slower | Faster |
| Strength | Mild–moderate | Moderate–high |
| Best for | Beginners, sensitive skin | Oily, acne-prone skin |
| Focus | Gradual texture improvement | Faster acne + texture results |
If your goal is faster improvement in clogged pores and uneven texture, retinal is usually the more efficient option — but only if your skin can tolerate it.
Both are vitamin A derivatives, but they behave differently once applied to the skin.
Retinol requires several conversion steps before becoming retinoic acid, which makes it slower and generally easier to tolerate. This makes it a reliable starting point for beginners or for skin that reacts easily to active ingredients.
Retinal (retinaldehyde) sits much closer to the active form. Because of this, it works more efficiently on cell turnover, which is why results often appear sooner — especially when it comes to smoothing texture, clearing pores, and improving post-acne marks (PIH).
For oily and acne-prone skin, this difference is important.
Faster conversion means a more direct effect on how the skin renews itself. As cell turnover improves, buildup inside the pore decreases, which leads to fewer clogged pores and more refined texture over time.
This is why retinal has become more popular in modern routines — it offers a middle ground between retinol and stronger prescription options.
However, faster doesn’t always mean better.
If your skin is reactive, easily irritated, or still adjusting to active ingredients, starting with retinol — or even adapalene — is often the more stable approach.
The goal isn’t speed.
It’s finding the level your skin can handle consistently without disruption.
Prescription vs OTC retinoids
The difference between OTC and prescription retinoids isn’t just strength — it’s how directly they deliver active vitamin A to the skin.
| Type | Examples | How they work | Strength level | Best for |
|---|---|---|---|---|
| OTC retinoids | Retinol, Retinal, Adapalene | Require conversion or are optimized for gradual release | Mild → Moderate | Beginners, oily skin, early–moderate acne |
| Prescription retinoids | Tretinoin, Tazarotene | Already active (retinoic acid) or very close to it | Moderate → High | Persistent acne, resistant congestion |
If your skin is still adjusting or prone to irritation, starting with OTC retinoids gives you more control — while prescription options are better suited when acne becomes more persistent or unresponsive.
OTC retinoids work more gradually. Ingredients like retinol and retinal need conversion inside the skin before becoming retinoic acid, which slows their effect and makes them easier to tolerate. Even adapalene, which is already active, is designed to be more stable and less irritating, making it a strong option for oily, acne-prone skin starting treatment.
Prescription retinoids, such as tretinoin and tazarotene, act more directly. Because they are already in or very close to the active form, they have a stronger impact on cell turnover, which can make them more effective for persistent acne — but also more likely to cause irritation if not introduced carefully.
In practice, the difference shows up in how your skin responds.
If your acne is mild to moderate, or your skin is still building tolerance, OTC retinoids are often enough to improve clogged pores, texture, and overall skin behavior when used consistently.
If breakouts continue despite a structured routine, or if congestion remains unchanged over time, prescription retinoids may offer the level of control needed to shift that pattern.
This isn’t about moving to something “stronger.”
It’s about choosing the level of precision and intensity your skin actually requires.
What makes a retinoid formula acne-friendly?
The effectiveness of a retinoid doesn’t depend on the ingredient alone — the formula determines whether your skin improves or breaks out.
For oily and acne-prone skin, texture matters more than most people realize.
A retinoid can be clinically effective, but if the formulation is too heavy or occlusive, it can sit on the skin in a way that contributes to clogged pores rather than preventing them. This is why lighter formats tend to work better.
Look for gel, serum, or fluid textures that are absorbed easily without leaving a thick layer behind. These are more compatible with how oily skin behaves and are less likely to interfere with natural sebum flow.
At the same time, “lightweight” doesn’t mean stripping.
One of the most common mistakes is using a retinoid without enough barrier support. When the skin becomes dehydrated, it often produces more oil to compensate — which can make breakouts feel worse, not better. This pattern is closely linked to dehydrated oily skin and how barrier disruption affects oil production.
A well-formulated retinoid should feel balanced on the skin.
It should support cell turnover without leaving the skin tight, irritated, or reactive. This is where pairing it with the right supporting products becomes essential — especially a lightweight moisturizer for oily acne-prone skin and a gentle cleanser that maintains the skin barrier without over-stripping.
The goal is not just to apply a retinoid.
It’s to create an environment where your skin can tolerate it consistently — because consistency is what allows retinoids to actually change how pores behave over time.
How to start using retinoids for oily, acne-prone skin
Retinoids tend to cause problems at the beginning not because they’re the wrong choice, but because they’re introduced too quickly for the skin to handle.
One of the most common mistakes isn’t choosing the wrong retinoid, but using the right one too aggressively. When you first begin, your skin isn’t used to increased cell turnover, and applying it every night can overwhelm it. This often shows up as irritation, tightness, or even more breakouts, which can make it feel like the product isn’t working, when in reality the skin just hasn’t had time to adapt.
Building tolerance: the 1/2/3 rule
A more gradual approach tends to work much better.
The 1/2/3 rule is a simple way to build tolerance without disrupting your skin. You start by using the retinoid once in the first week, then twice in the second, and three times in the third. After that, the frequency should be guided by how your skin responds to it.
What makes the real difference is not how fast you increase usage, but whether your skin can stay consistent with it over time.
Application: how to apply retinoids correctly

A retinoid should always be applied to completely dry skin, as damp skin increases absorption and can make irritation more likely, especially early on. The amount matters as well — a pea-sized amount is enough for the entire face. Using more won’t improve results; it usually just increases sensitivity without adding any benefit.
The “sandwich method” and barrier protection
When you start using a retinoid, it’s common for the skin to feel tight while still looking oily, which can be confusing at first. This usually isn’t a sign that the product isn’t working, but rather that the skin barrier is struggling to keep up with the increase in cell turnover.
A simple way to make this transition easier is the sandwich method, where you apply moisturizer before and after your retinoid. Instead of applying it directly to bare skin, you use a light layer of moisturizer first, then the retinoid, followed by another layer of moisturizer.
This doesn’t reduce the effectiveness of the retinoid. It simply slows down how quickly it penetrates, which helps minimize irritation and makes the process more tolerable.
When to use the sandwich method
This approach is especially helpful if your skin tends to feel reactive, or if it becomes tight but continues to break out — a pattern often linked to dehydrated oily skin and how barrier imbalance affects oil production.
It’s also useful during the first few weeks, when your skin is still adjusting and more likely to become irritated.
Over time, as your skin builds tolerance, you may find that you no longer need to buffer it in the same way.
Retinization timeline: how long it takes to work
Retinoids don’t change your skin overnight. What they do is gradually shift how your skin behaves, and that process takes time.
This adjustment phase is known as retinization, and for most people it lasts somewhere between 4 to 12 weeks.
During this period, your skin is adapting to increased cell turnover, which can temporarily affect how it looks and feels. You might notice some dryness, mild flaking, or small breakouts appearing more quickly than usual.
This can feel discouraging, especially early on, but it’s part of how the skin resets its rhythm.
What matters is not what happens in the first couple of weeks, but how your skin changes over time. As the adjustment phase passes, breakouts tend to become less frequent, pores stay clearer for longer, and overall texture becomes more even.
Consistency during this phase is what allows those changes to happen.
Purging vs irritation: how to tell the difference
When breakouts appear after starting a retinoid, it’s easy to assume something is going wrong. In reality, not all reactions mean the same thing.
A skin purge happens when increased cell turnover brings existing microcomedones to the surface faster. These are clogs that were already forming under the skin, and the retinoid simply speeds up their appearance.
This usually shows up in areas where you normally break out, and the spots tend to resolve more quickly than usual.
Irritation, on the other hand, feels different.
It often shows up as redness, burning, or sensitivity, sometimes accompanied by breakouts in areas that don’t usually react. Instead of improving over time, it tends to persist or worsen if the routine stays the same.
If it’s purging, the best approach is to stay consistent and give your skin time to adjust. If it’s irritation, it’s a sign to slow down — reduce frequency, support the barrier, and allow your skin to recover before increasing again.
How to combine retinoids with other acne treatments
Using a retinoid alongside other treatments can be very effective, but only when the routine is structured in a way your skin can handle.
Trying to use multiple active ingredients in the same routine often leads to irritation rather than better results. A more balanced approach is to alternate them across different nights, allowing each ingredient to work without overwhelming the skin.
Alternating active nights
A simple structure might look like using your retinoid one night, an exfoliating ingredient like BHA on another, and leaving space in between for recovery. This gives your skin time to reset while still addressing different aspects of acne.
This kind of rhythm becomes much easier to maintain when it’s part of a structured night routine rather than something you try to adjust day by day.
Over time, this approach tends to be more effective than layering everything at once, because it keeps the skin stable — and stability is what allows long-term improvement.
A note on sun exposure and retinoids
Using a retinoid without proper sun protection is one of the easiest ways to disrupt your progress, even if your routine is otherwise correct.
After using retinol consistently for around six months, I started to see clear improvements in my skin — smoother texture, more even tone, and fewer recurring breakouts. The only issue came later, when I underestimated how much sun exposure would affect my skin. Even though I had stopped using it right before summer and was applying sunscreen, the combination of heat and prolonged sun still led to sensitivity that took time to fully recover from.

That experience didn’t change the value of retinoids, but it did change how I use them.
Being more mindful during periods of intense sun — whether that means reducing frequency, reinforcing sunscreen, or choosing a non-comedogenic sunscreen for oily and acne-prone skin that protects without clogging pores — makes a noticeable difference in how well your skin tolerates them long term.
Final takeaway: what actually makes retinoids work
Retinoids don’t work because they’re strong.
They work because they change how your skin behaves over time.
For oily and acne-prone skin, the real shift happens when cell turnover, oil flow, and pore behavior become more stable. That’s what reduces recurring clogs, not just treating breakouts as they appear.
The difference comes from how you use them.
Starting gradually, supporting the skin barrier, and staying consistent matters far more than choosing the strongest formula. When retinoids are used in a way your skin can tolerate, they become one of the most reliable tools for long-term skin clarity.
Frequently Asked Questions
Which retinol is best for oily, acne-prone skin?
For oily and acne-prone types, Retinaldehyde (Retinal) or Adapalene are the top choices. Unlike standard retinol, Retinal has unique antibacterial properties that directly target acne bacteria, while Adapalene was specifically designed to treat the “sticky” cells inside the pore that lead to follicular hyperkeratosis.
What is the 1/2/3 rule for retinol?
The 1/2/3 rule is a titration schedule used to minimize purging and irritation:
Week 1: Apply your retinoid 1 night only.
Week 2: Apply 2 nights (spaced out).
Week 3: Apply 3 nights (every other day). By week 4, if your barrier feels strong, you can gradually move toward daily use.
Is 1% retinol too strong for beginners?
Yes, a 1% retinol concentration is considered high-strength and often leads to “retinol burn” for beginners. If you are just starting, it is much safer to begin with a 0.3% retinol or a 0.05% retinal. For oily skin specifically, a non-comedogenic retinol serum with a lower percentage will yield better long-term results than a high-strength cream that causes peeling.
What works 11 times faster than retinol?
Retinaldehyde (Retinal) works 11 times faster than traditional retinol because it only requires one conversion step to become retinoic acid in the skin. This makes it 3 times more effective for clearing deep clogs and improving the appearance of acne scars compared to standard over-the-counter retinol.
What do Koreans use instead of retinol?
In K-beauty, many people with sensitive or dehydrated oily skin use Bakuchiol or Ginseng-derived Vitamin A precursors. Bakuchiol is a plant-based alternative that offers similar pore-refining benefits without the risk of retinization or sun sensitivity, making it a popular choice for those who find traditional retinoids too harsh.
Is 25 too late to start retinol?
Absolutely not. In fact, 25 is often considered the “sweet spot” for starting. At this age, natural collagen production begins to slow, and using a retinoid can help manage late-twenties “adult acne” while acting as a preventative measure for fine lines. It is a long-game ingredient that pays off significantly over time.
Can I use a retinoid every day?
You can use a retinoid every day once your skin has fully acclimated, which typically takes 4–12 weeks. However, many people with oily skin find that “Micro-dosing”—using it 4 to 5 nights a week—is enough to maintain clear pores while allowing them to use a salicylic acid face wash on off-nights for surface oil control.
What is the strongest retinoid?
The strongest retinoid available is Tazarotene, followed by Tretinoin. These are prescription-strength medications used for severe acne and deep structural skin repair. While they are highly effective, they also carry the highest risk of a compromised barrier and require a strict night skin care routine including a high-quality moisturizer for oily skin.
Sources and References
- DermNet NZ. Topical retinoids: Vitamin A derivatives and their role in regulating skin renewal and acne treatment.
Available at: https://dermnetnz.org/topics/topical-retinoids - American Academy of Dermatology (AAD). Acne clinical guideline: Recommendations for topical retinoids as a core treatment for acne-prone skin.
Available at: https://www.aad.org/member/clinical-quality/guidelines/acne - American Academy of Dermatology (AAD). Guidelines of care for the management of acne vulgaris. Published in the Journal of the American Academy of Dermatology (JAAD).
Available at: https://www.jaad.org/article/S0190-9622(23)03389-3/fulltext - Journal of Clinical and Aesthetic Dermatology. Why Topical Retinoids Are Mainstay of Therapy for Acne.
Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC5574737/
This article is based on dermatology research and peer-reviewed studies on acne pathogenesis, hormonal signaling, and skin barrier function.
Medical Disclaimer
Gentle Glow guides are developed using peer-reviewed dermatology research and established clinical guidelines. The information provided is for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. Always consult a board-certified dermatologist or qualified healthcare provider before starting new active skincare treatments.



