Medically reviewed • Updated March 2026 • Evidence-based skincare
Many people believe acne happens simply because their skin produces too much oil. It’s a common assumption — if the face looks shiny, the oil must be causing the breakouts. But dermatology research shows that oil alone rarely causes acne. Breakouts develop when excess sebum combines with dead skin cells and bacteria inside the pore, creating the conditions for inflammation.
What makes this process more interesting is that it doesn’t happen randomly. Acne formation often follows a daily biological rhythm influenced by hormones, oil production, and microbial activity. Understanding this bio-adaptive cycle — how your skin’s oil and bacteria change throughout the day — helps explain why pores clog, why breakouts often appear overnight, and why managing oily skin requires more than simply washing the face.
If you’re still learning how excess oil, breakouts, and barrier damage connect, start with our complete guide to how oily and acne-prone skin works.
ⓘ Dermatology Note
Why oily skin develops acne
Acne on oily skin develops when several biological processes occur at the same time. Sebaceous glands produce sebum to protect and lubricate the skin, but when excess oil mixes with dead skin cells inside the hair follicle, it forms a blockage. This clogged pore creates a low-oxygen environment where Cutibacterium acnes bacteria multiply. As the immune system reacts to trapped bacteria and oxidized oil, inflammation develops, producing the visible pimples, blackheads, and whiteheads associated with acne.
What Causes Acne on Oily Skin?
Understanding what causes acne on oily skin begins with several biological processes happening inside the pore. Sebaceous glands produce sebum to protect and lubricate the skin, but when excess oil mixes with dead skin cells inside the hair follicle, it forms a blockage.
Oily skin produces larger amounts of sebum from sebaceous glands. When this oil combines with shed skin cells inside the pore, it forms the earliest stage of acne known as a microcomedone. Over time, trapped oil can oxidize, bacteria multiply, and the immune system responds with inflammation. This chain reaction inside the pore is what ultimately produces the acne lesions that appear on the skin’s surface.
In reality, acne formation is not a single event but a sequence of biological changes happening inside the pore throughout the day. Hormones stimulate oil production in the morning, sebum levels peak around midday, and the oil on the skin begins to oxidize as it interacts with oxygen and environmental stressors. By nighttime, bacteria inside clogged pores multiply more easily, which is why many people notice that new breakouts seem to appear overnight.
Understanding this timeline reveals an important insight: acne on oily skin is not simply about oil, but about timing, chemistry, and microbial activity inside the pore. Dermatologists increasingly recognize that acne development follows a predictable rhythm — one that becomes clearer when we look at the skin across a full 24-hour cycle.
Table of Contents
Quick Summary: How Acne Forms Inside the Pore
| Acne Trigger | What Happens in the Pore |
|---|---|
| Excess sebum | Oil fills the follicle and mixes with dead skin cells |
| Hyperkeratinization | Sticky skin cells form a microscopic plug |
| Bacterial growth | C. acnes multiplies inside the clogged pore |
| Inflammation | The immune system reacts, producing visible pimples |
The 24-Hour Acne Timeline

Acne on oily skin doesn’t usually form in a single moment. Instead, it develops through a sequence of biological changes that unfold throughout the day inside the pore. Hormones influence oil production in the morning, sebum levels rise toward midday, and the oil on the skin begins to oxidize as it interacts with oxygen and environmental stressors. By nighttime, bacteria inside clogged pores multiply more easily.
Understanding this daily rhythm helps explain a pattern many people notice but rarely understand: skin that looks relatively calm in the morning can become noticeably oilier by midday, while new breakouts often appear the next morning.
08:00 AM — The Cortisol Kickstart
When we wake up, the body experiences a natural increase in cortisol known as the cortisol awakening response. This hormone helps regulate alertness and metabolism, but it also influences the sebaceous glands.
Sebaceous glands respond to hormonal signals by increasing oil production. For people with oily skin, this means the day often begins with the first surge of sebum moving through the pores. While this oil is part of the skin’s natural protection system, it also begins setting the stage for potential pore congestion later in the day.
This early hormonal signal is one reason why managing oily skin often starts with a balanced morning routine, designed to remove excess oil without disrupting the skin barrier.
11:00 AM — The Sebum Peak
Around late morning to midday, many people experience the peak of sebum excretion rate (SER). This is the moment when sebaceous glands are releasing the highest amount of oil onto the skin’s surface.
If you’ve ever looked in the mirror around lunchtime and noticed that your skin suddenly appears shiny, this is likely the result of that midday oil peak. The sebum itself is not harmful, but when larger amounts of oil mix with naturally shedding skin cells inside the pore, the combination can begin forming the earliest stage of a blockage.
Dermatologists refer to this stage as a microcomedone — a tiny plug of oil and skin cells that forms deep within the follicle before any visible acne appears.
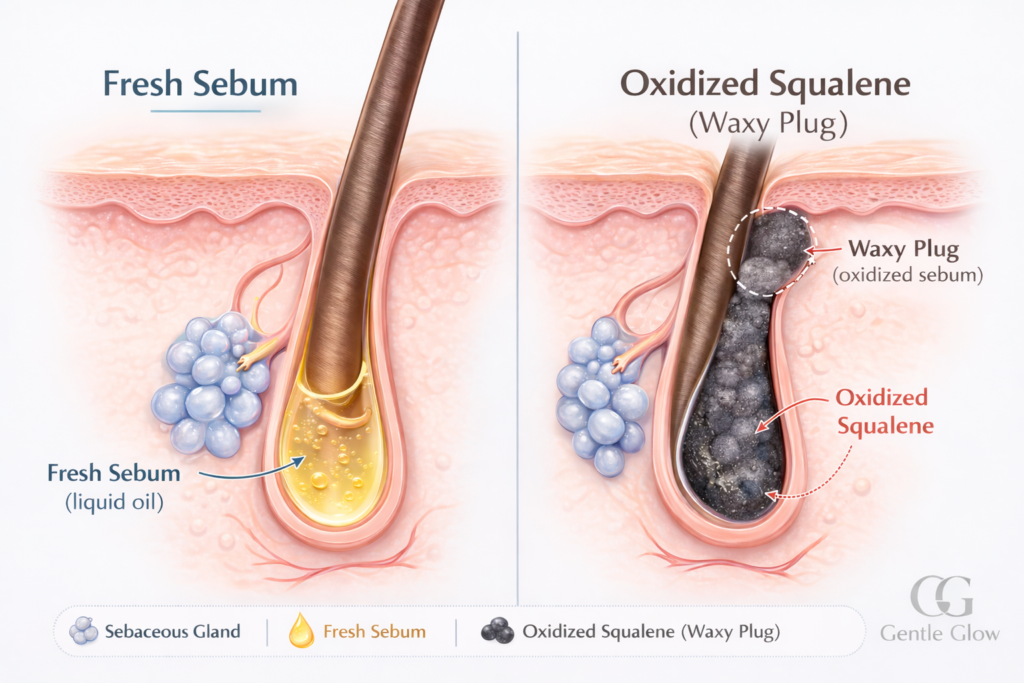
04:00 PM — The Oxidation Window
As oil sits on the skin throughout the afternoon, it begins interacting with oxygen in the air and environmental stressors such as pollution and UV exposure. This process can trigger sebum oxidation, particularly affecting a lipid called squalene, a reaction that has been studied in dermatology research examining how oxidized sebum contributes to acne inflammation, including studies published in journals such as MDPI Dermatology Reports.
A helpful way to imagine this process is to think about how metal slowly rusts when exposed to air. In a similar way, certain components of skin oil can chemically change when exposed to oxygen, becoming more irritating to the surrounding skin.
When oxidized oil remains trapped inside a clogged pore, it can contribute to inflammation and darkened pore contents — one reason blackheads often appear darker on the surface of the skin.
How to Spot Sebum Oxidation in the Mirror
Sebum oxidation is often visible as darkened sebaceous filaments or blackheads on areas like the nose, chin, and forehead. These spots may appear as tiny gray or black dots inside the pore opening.
While they are often mistaken for dirt, their darker color is usually the result of oil that has reacted with oxygen rather than debris sitting on the skin.
10:00 PM — The Biofilm Bloom
By nighttime, the environment inside a clogged pore becomes more favorable for bacterial growth. The bacterium Cutibacterium acnes thrives in the low-oxygen conditions created by trapped oil and skin cells.
As these bacteria multiply, they can begin forming a protective structure known as a biofilm. A helpful analogy is plaque on teeth. Just as plaque forms a sticky layer that protects bacteria on the surface of teeth, biofilms can create a shield that allows acne bacteria to persist inside the pore.
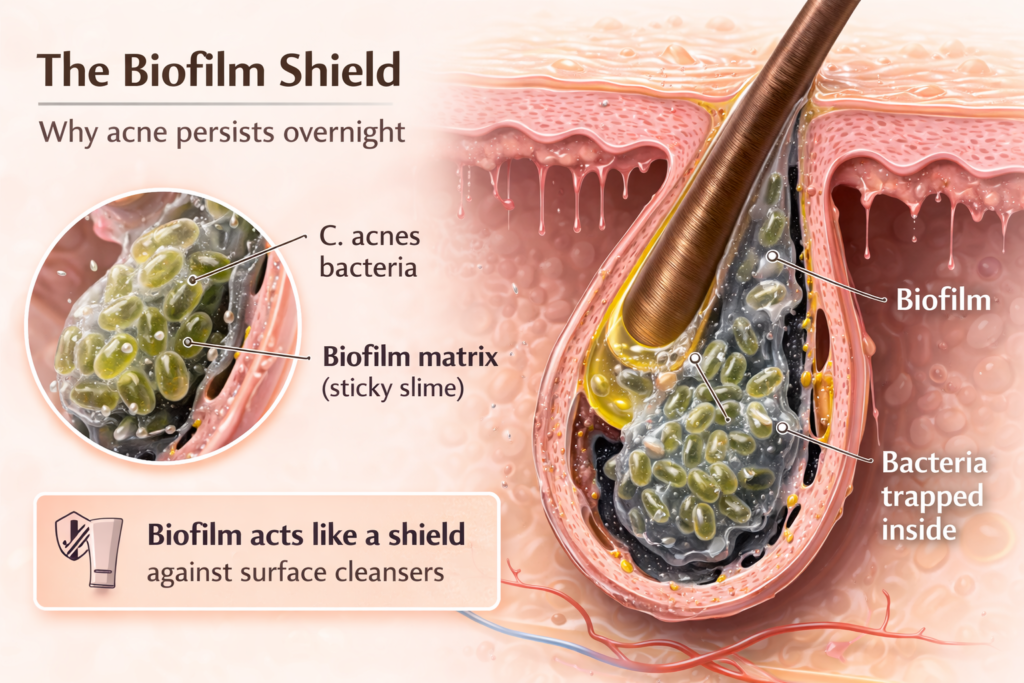
Because of this protective layer, simple cleansing at the surface of the skin does not always remove the deeper biological processes that contribute to acne formation. Over time, the immune system reacts to the bacteria and trapped oil, leading to redness, swelling, and the visible pimples many people notice the following morning.
Why Breakouts Often Appear Overnight
This nighttime bacterial activity explains a common experience: going to bed with relatively calm skin and waking up with a new pimple. While the inflammation becomes visible in the morning, the underlying biological processes have usually been developing inside the pore for many hours.
Acne formation is therefore less about a single trigger and more about a daily cycle of oil production, oxidation, and microbial activity that gradually transforms a clogged pore into an inflamed breakout.
Beyond Clogged Pores: The Hidden Causes of Acne
Oil and bacteria are often blamed for acne, but dermatology research shows that breakouts depend on several biological processes happening inside the pore at the same time. While excess sebum creates the environment for clogged pores, other factors — including how skin cells behave, how the microbiome shifts, and how well the skin barrier holds moisture — determine whether a pore remains stable or becomes inflamed.
Understanding these hidden mechanisms explains why some people with oily skin rarely experience breakouts, while others develop persistent acne even when they follow careful skincare routines.
Sticky Skin Cells: Follicular Hyperkeratinization
One of the earliest stages of acne begins when the skin’s natural shedding process becomes irregular. Normally, dead skin cells detach from the follicle and move to the surface without blocking the pore. But in acne-prone skin, these cells can become unusually sticky.
Dermatologists call this process follicular hyperkeratinization. Instead of shedding smoothly, the cells clump together with oil, forming the first microscopic blockage inside the pore. This tiny plug, known as a microcomedone, can later develop into blackheads, whiteheads, or inflamed pimples.
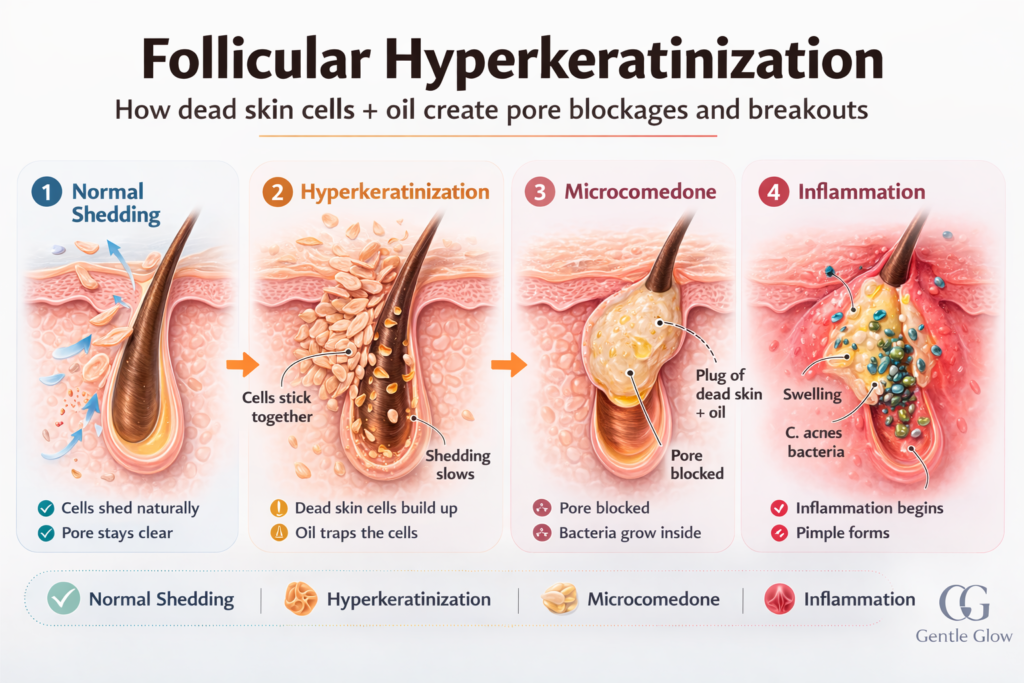
When acne becomes inflamed, dermatologists often recommend treatments like benzoyl peroxide or BHA exfoliants. Understanding how salicylic acid and benzoyl peroxide treat acne can help you choose the right option.
Microbiome Imbalance Inside the Pore
Not all Cutibacterium acnes bacteria behave the same way. Human skin naturally contains a complex microbiome — a community of microorganisms that normally coexist without causing inflammation.
In acne-prone skin, however, certain strains of C. acnes can become dominant. These strains produce inflammatory byproducts that irritate the surrounding skin and trigger the immune response responsible for red, swollen pimples.
When this imbalance occurs inside a clogged pore, bacteria can also form protective biofilms that make them more resistant to simple surface cleansing. This is why acne treatment often focuses on ingredients that can penetrate the pore and disrupt bacterial activity.
The Dehydration Paradox
Another hidden factor in oily acne-prone skin is barrier dehydration. Many people try to control oil by using harsh cleansers, strong toners, or frequent exfoliation. While this may temporarily reduce shine, it can also weaken the skin’s protective barrier.
When the barrier loses water, the sebaceous glands may respond by producing even more oil in an attempt to protect the surface of the skin.
If your skin feels like it’s shrinking but looks like a mirror by noon, you aren’t crazy — you’re likely dealing with reactive seborrhea, a condition where dehydration triggers increased oil production.
This paradox explains why some people experience both tightness and excess shine at the same time, a common pattern in oily dehydrated skin.
Lifestyle Triggers That Can Worsen Acne
While acne begins inside the pore, certain lifestyle factors can intensify the process. Stress hormones can stimulate sebaceous glands, heat and humidity may increase oil production, and friction from helmets, phones, or tight clothing can irritate the skin.
Diet can also play a role in some individuals. Foods that rapidly raise blood sugar levels may stimulate the release of insulin and related hormones, which can indirectly increase oil production.
The Sugar–Acne Connection
Instead of focusing on a single “acne-causing food,” dermatologists often look at the glycemic load of the diet. Highly refined carbohydrates and sugary foods can cause rapid spikes in blood sugar, which may stimulate hormonal pathways linked to oil production and acne development, a relationship explored in dermatology research indexed by the National Institutes of Health.
For some people, this connection between blood sugar and oil production can make breakouts more likely, particularly when combined with other factors such as clogged pores and bacterial growth.
Understanding the biological causes of acne helps explain an important point: oily skin itself is not the enemy. Breakouts occur when several processes — oil production, skin cell buildup, bacterial activity, and inflammation — interact inside the pore.
The goal of effective skincare is therefore not to eliminate oil completely, but to regulate it while keeping pores clear and supporting the skin barrier.
Next, we’ll look at how to control acne on oily skin without disrupting the balance that healthy skin needs.
How to Control Acne on Oily Skin
Understanding the causes of acne is important, but it also reveals something reassuring: oily skin itself is not the enemy. Breakouts occur when excess oil combines with sticky skin cells, bacteria, and inflammation inside the pore. Managing acne therefore focuses on regulating these processes rather than trying to eliminate oil completely.
A balanced skincare routine usually begins with gentle cleansing, which removes excess oil and environmental debris without stripping the skin barrier. When the barrier remains healthy, the skin is less likely to respond with reactive oil production.
Exfoliation also plays a role, particularly with ingredients such as salicylic acid (BHA). Because BHA is oil-soluble, it can travel inside the pore and help dissolve the mixture of oil and dead skin cells that leads to clogged follicles.
Oil-regulating ingredients like niacinamide can further support acne-prone skin by helping balance sebum production while calming inflammation. Combined with lightweight moisturizers and non-comedogenic sunscreen, these steps help maintain the delicate balance between controlling oil and protecting the skin barrier.
Common Skincare Mistakes That Can Make Acne Worse
Many people with oily skin attempt to control breakouts by aggressively removing oil. Ironically, this approach can often make acne worse. Understanding what causes acne on oily skin helps explain why managing oil alone is not enough to prevent breakouts.
Frequent scrubbing or harsh cleansers can damage the skin barrier, causing the skin to lose water. When this happens, sebaceous glands may compensate by producing even more oil — the same reactive cycle that contributes to the dehydration paradox discussed earlier.
Over-exfoliation is another common issue. While chemical exfoliants can help clear pores, using them too frequently may irritate the skin and increase inflammation. In acne-prone skin, irritation can make existing breakouts appear more severe.
Skipping moisturizer is another mistake many people make when trying to control oil. In reality, properly hydrated skin is often less likely to overproduce sebum, which is why lightweight, oil-free moisturizers are recommended even for very oily skin types.
Conclusion
Acne on oily skin is not simply the result of excess oil. Breakouts develop through a complex chain reaction involving sebum production, sticky skin cells, bacterial activity, and inflammation inside the pore.
When these factors interact over time, a clogged pore can gradually evolve into an inflamed pimple. Understanding this process — and the daily rhythm that influences oil production and bacterial growth — helps explain why acne often appears unpredictable.
Understanding what causes acne on oily skin makes it easier to control breakouts without damaging the skin barrier.
Rather than trying to eliminate oil completely, effective skincare focuses on regulating sebum, keeping pores clear, and protecting the skin barrier. With the right approach, even oily skin can remain balanced while the frequency and severity of breakouts gradually improve.
Frequently Asked Questions
What causes acne on oily skin?
Acne is caused by a combination of excess sebum, “sticky” dead skin cells (hyperkeratinization), and the growth of C. acnes bacteria inside an oxygen-deprived pore.
How to 100% remove pimples?
While you cannot “cure” acne permanently, you can control it by regulating oil production, preventing sebum oxidation, and supporting your skin barrier. Consistency is more effective than “spot treating” after a breakout appears.
Does Accutane help with oily skin?
Yes. Accutane (Isotretinoin) works by physically shrinking the sebaceous glands, which permanently reduces oil production. However, it is a serious medical treatment and should only be discussed with a dermatologist.
What acid is best for acne?
Salicylic Acid (BHA) is the gold standard for oily skin because it is oil-soluble, allowing it to penetrate deep into the pore to dissolve clogs.
What foods cause acne?
High-glycemic foods (sugar, white flour, processed snacks) spike insulin, which triggers the IGF-1 pathway and increases oil production. Many people searching for what causes acne on oily skin are surprised to learn that oil alone isn’t responsible. Dairy can also be a trigger for some individuals due to natural growth hormones.

About the Author
Founder, Gentle Glow | Evidence-Based Skincare & Skin Biology
Hi, I’m the Founder of Gentle Glow. After years of struggling with oily and acne-prone skin—and cycling through harsh products that disrupted my barrier rather than improving it—I began researching the science behind sebum regulation, skin biology, and non-comedogenic formulation.
Gentle Glow was created to simplify evidence-based skincare. Every routine shared here focuses on root causes: barrier function, oil balance, and ingredient compatibility. My goal is to translate dermatology-backed principles into realistic, sustainable routines that work with your skin—not against it.
Beyond topical care, I believe healthy skin reflects overall balance, including nutrition, climate awareness, and lifestyle habits. Gentle Glow is built to help you make informed decisions with clarity, consistency, and confidence.
Medical Disclaimer
Gentle Glow guides are developed using peer-reviewed dermatology research and established clinical guidelines. The information provided is for educational purposes only and does not replace professional medical advice, diagnosis, or treatment. Always consult a board-certified dermatologist or qualified healthcare provider before starting new active skincare treatments.
Sources and References
- Acne: Symptoms and Causes — Mayo Clinic https://www.mayoclinic.org/diseasesconditions/acne/symptoms-causes/syc-20368047
- Squalene Peroxidation and Biophysical Parameters in Acne-Prone Skin: A Pilot “In Vivo” Study — MDPI https://www.mdpi.com/1424-8247/16/12/1704
- Dietary Glycemic Load and Acne Vulgaris — PubMed / NIH https://pubmed.ncbi.nlm.nih.gov/17616769/




